Problem Statement:
COVID19 is and will exhaust the current inventory of mechanical ventilators. While new units are being made, the idea to split a ventilator or co-vent has been tested and approved by FDA under an EAU (emergency authorization use).
The US posted this a few days ago: https://www.hhs.gov/sites/default/files/optimizing-ventilator-use-during-covid19-pandemic.pdf
This shows how it's possible, and approved in an emergency, to co-vent multiple patients. One of the challenges is making sure each patient has the right tidal volume at the right pressures. The ventilator, operating in pressure control mode, will control pressure and the breathing circuit and lung compliance will determine tidal volume into each set of lungs. But there is no method to easily measure individual tidal volume.
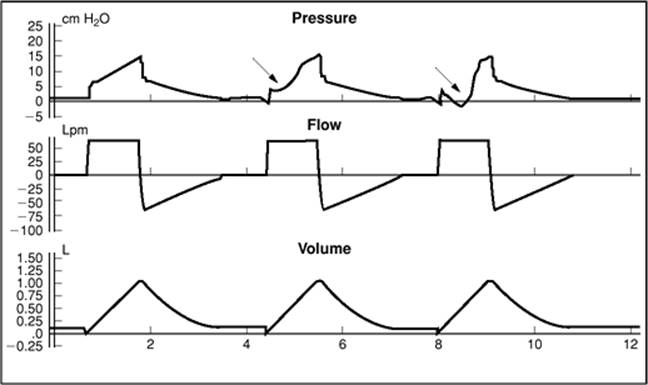
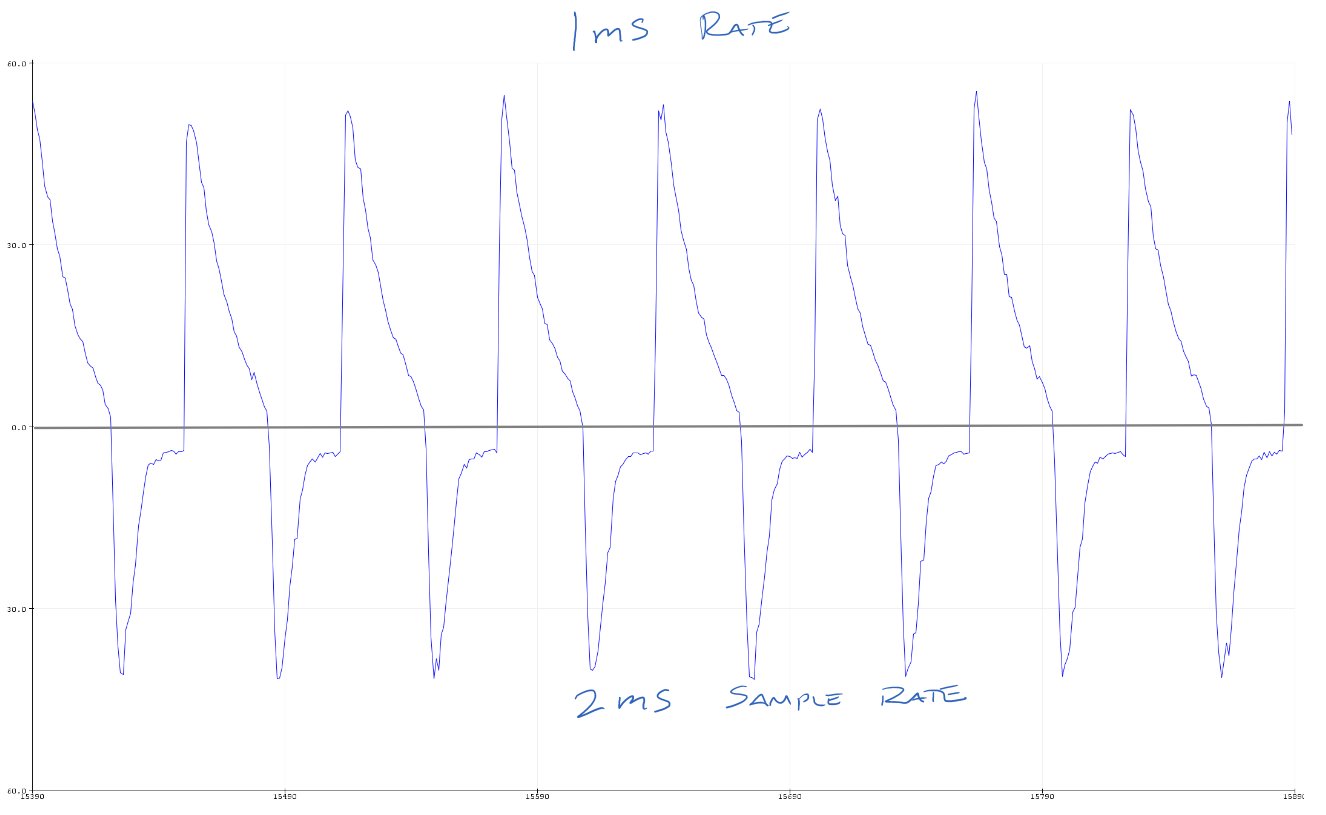
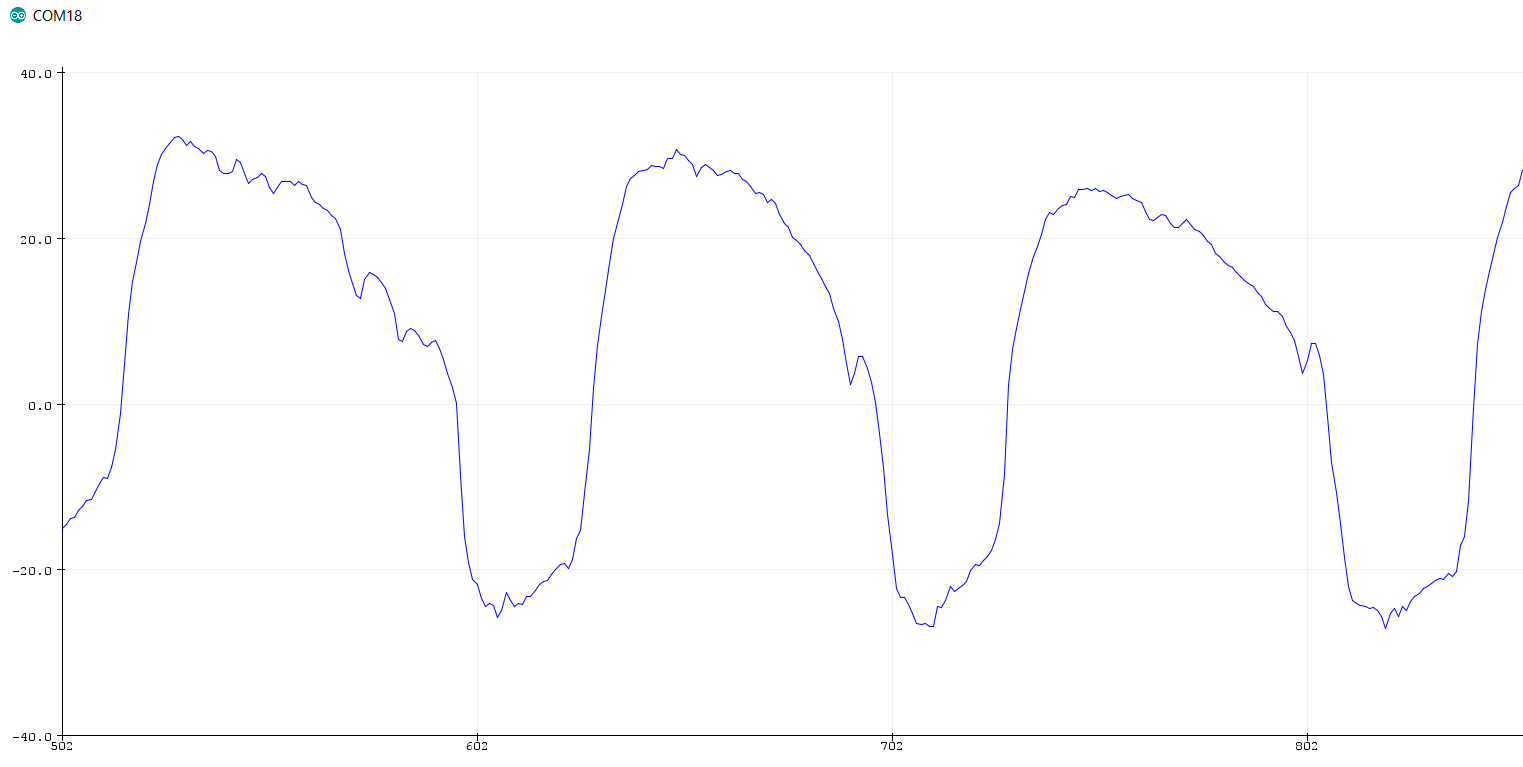
This chart shows typical pressure, flow and volume plots over time in seconds. The waveforms will be different for the settings on the ventilators and likely different for different manufacturers.
Aims:
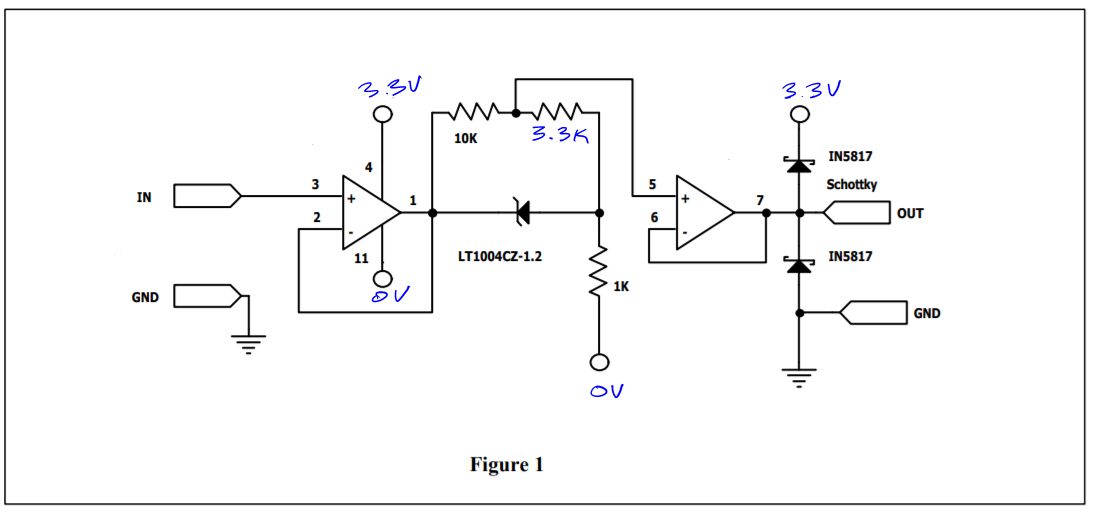
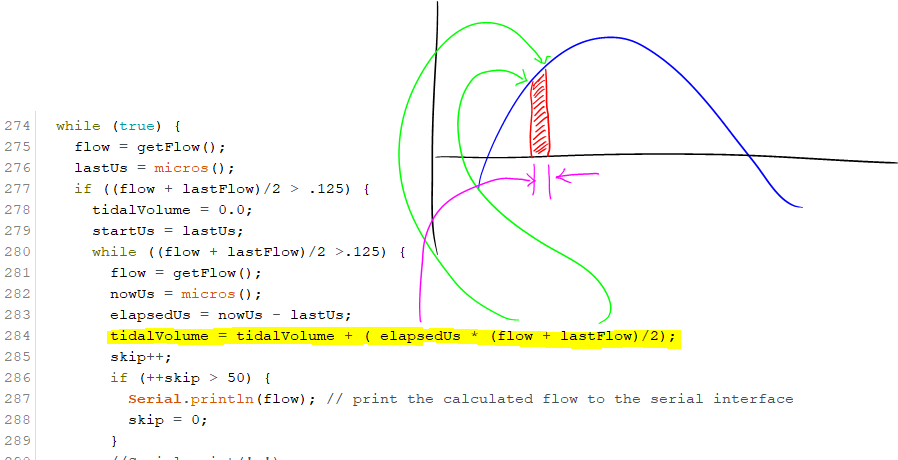
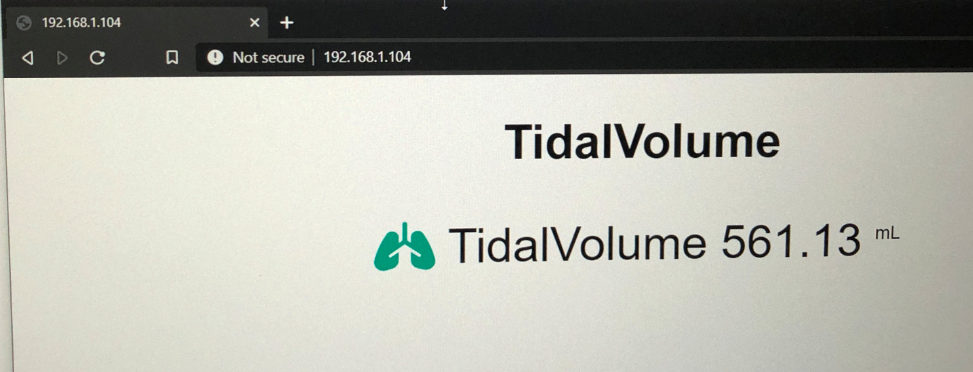
My focus is to create a TV meter as fast as possible so we can start to test. I eliminated the constraints of measuring pressures, BOM cost, part availability and regulatory compliance so I could create a test device and share knowledge with others, who are working on a similar device that don't ignore these constraints.
The final design, most likely someone's design, but possibly a fork of this design, will have pressure sensor for PIP & PEEP readout and buzzers and LED for alarms.
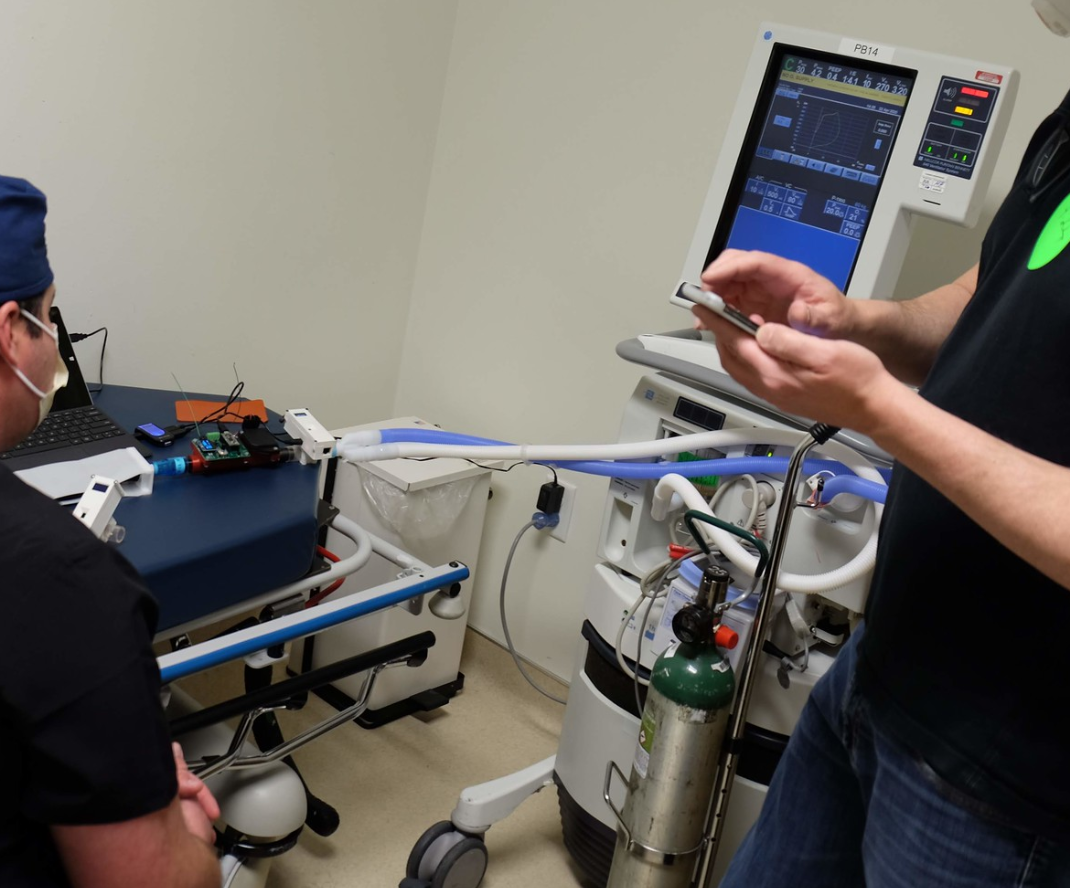
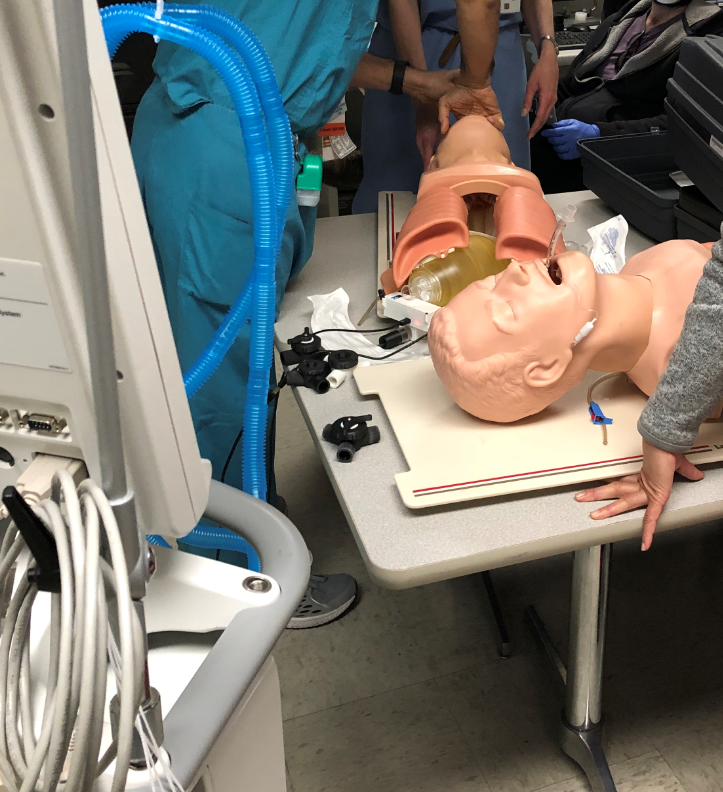
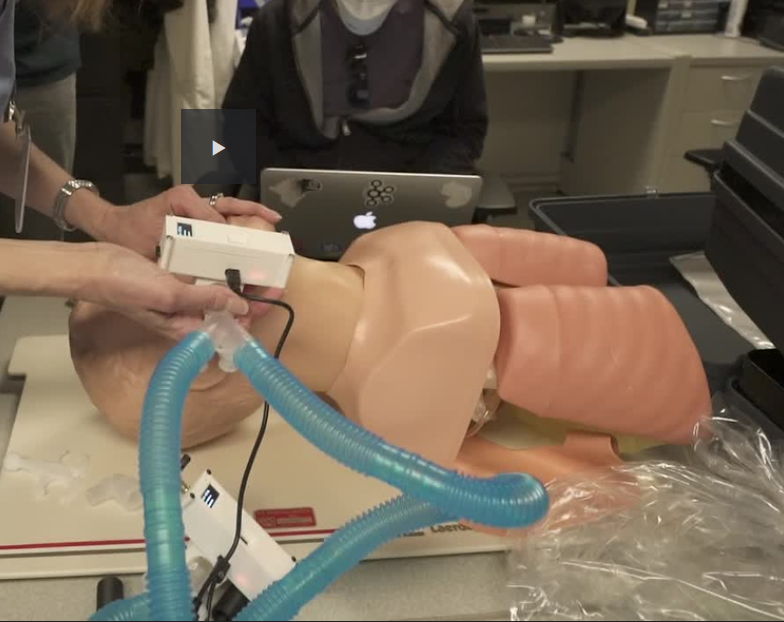
There is no intention on using this device on actual people, we will be testing it in a local lung lab at a medical school.
 Patrick
Patrick
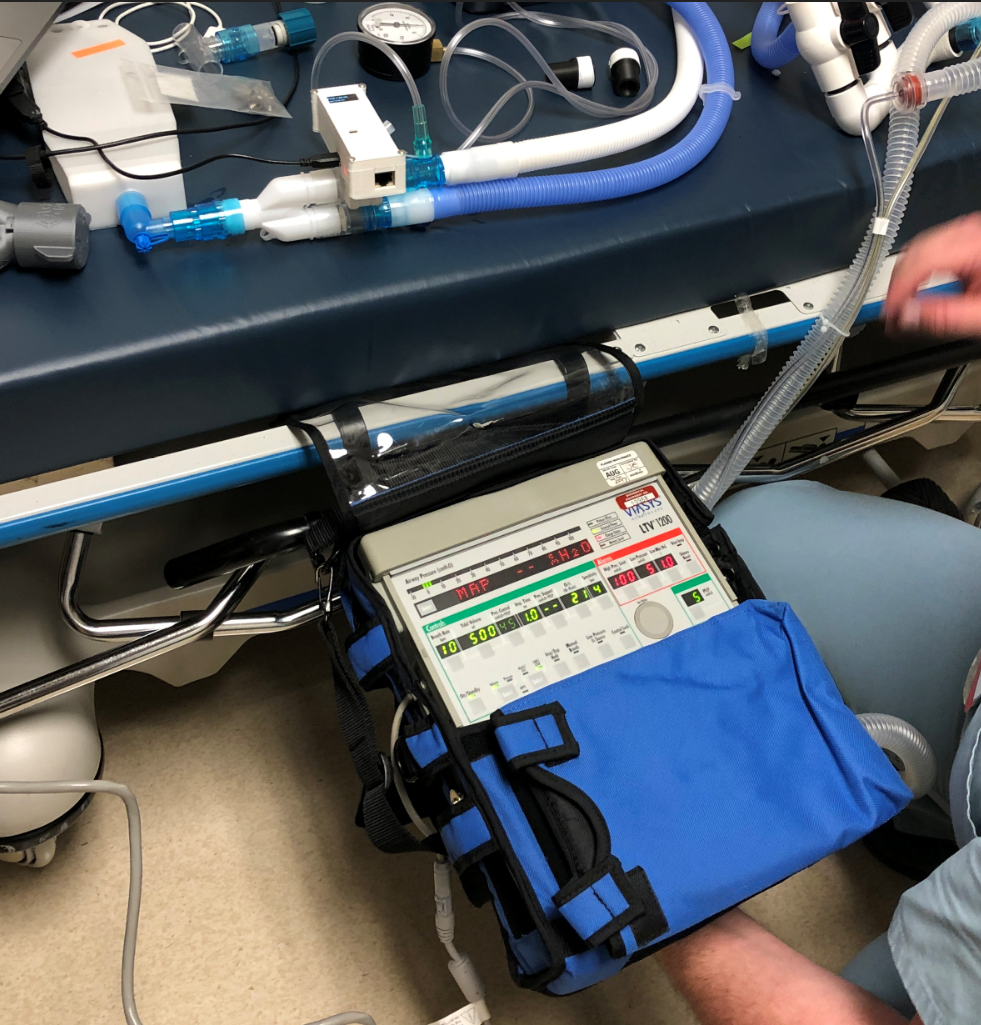
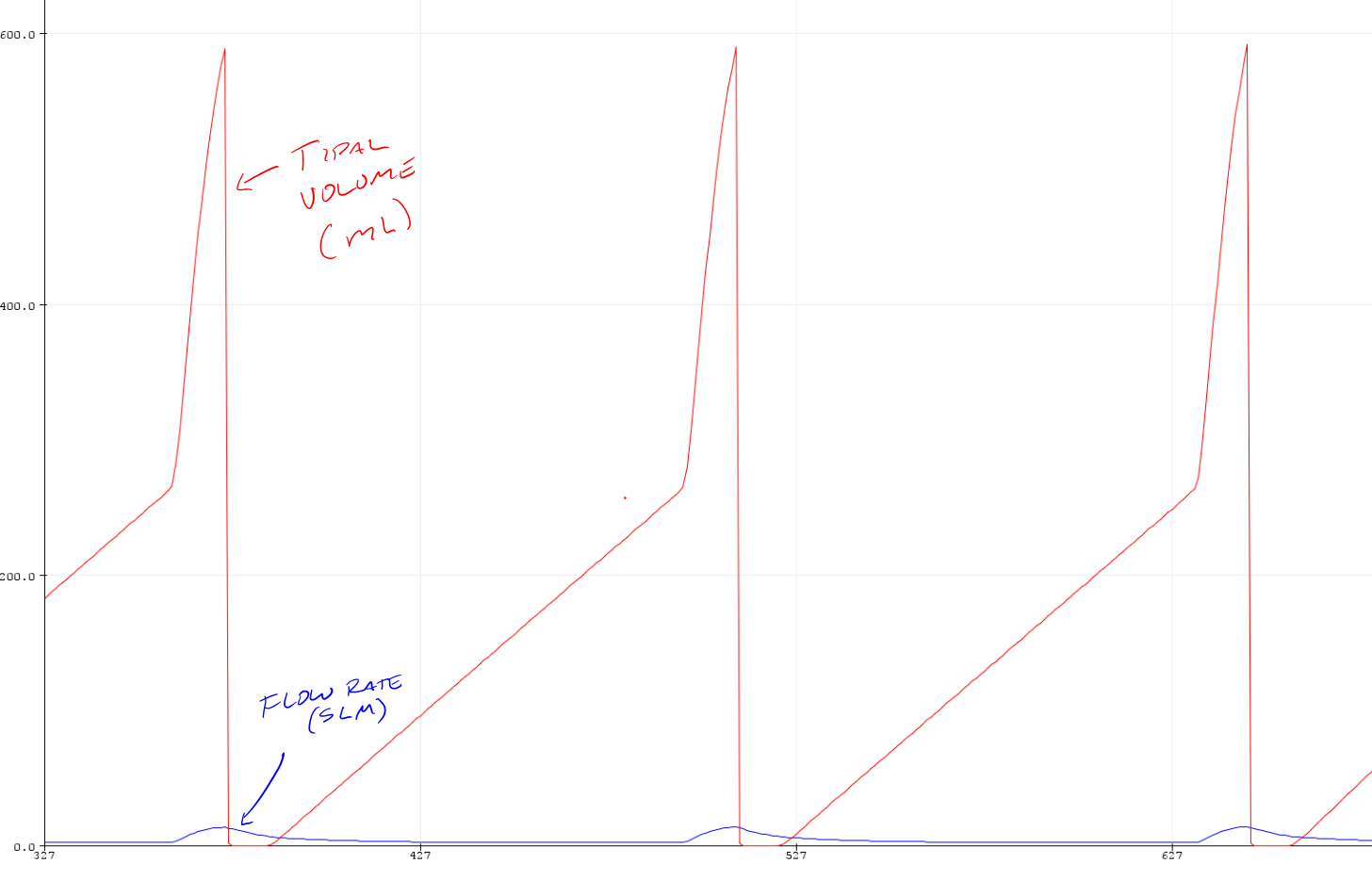
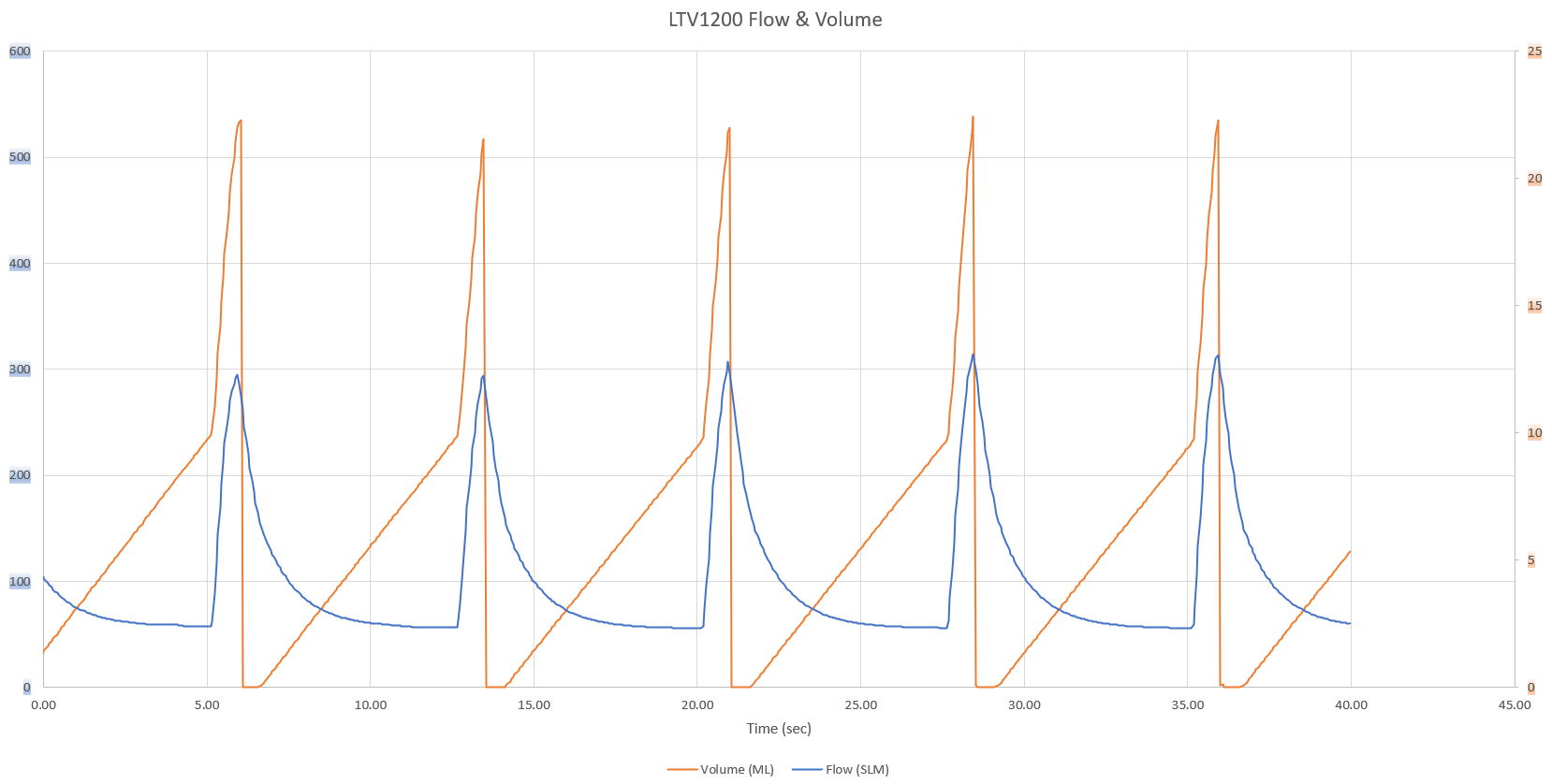















 Daren Schwenke
Daren Schwenke
 Mike Teachman
Mike Teachman
 pastcompute
pastcompute
 Craig Watson
Craig Watson
try the link on here: https://github.com/helpfulengineering/resources