You don’t drink? You die!
Dehydration (the lack of water within the body) is a serious threat. You may feel thirsty if your body wants to get hydrated, but your grandma probably doesn’t. As the feeling of thirst decreases with age, the need of water intake rises, due to reduced kidney functionality and more medication which needs to get washed out of the body. High demand of water with low liquid intake = problem. In in 2015, in Germany alone 100.764 people, mostly older than 70, got hospitalized with the primary diagnosis “acute dehydration”, leading to direct costs of more than 275 mio. € for the health system. Not speaking of the > 5000 deaths, and all the suffering and costs related to the possible implications of dehydration: paradox diarrhea, fall, cardiovascular diseases, kidney malfunction.
Why doesn’t anybody do something against dehydration?
Well, people do. Risk patients are monitored with a so-called hydration protocols, a table where the nurse notes down the volume of drinks given to the person of concern, a daily sum is calculated and – if too little was drunk – alarms are raised.
The problem with this approach: it takes the nurse some minutes every day. Time in nursing homes is expensive, and for that reason hydration-protocols are usually not applied in all, but only few cases of higher risk. But it is not these high-risk cases, which result in all these deaths and millions of costs. It’s the sum of those individuals, who are not monitored.
Solving the problem by automation
If in the current state of care liquid intake is not monitored because of the additional time needed for this task, then there is the need to automate fluid intake monitoring.
In other words: we want to minimize the time of human interaction needed for this task. Today, human interaction is needed in two major categories of liquid intake monitoring:
- Measurement of volume: the caregiver estimates/measures the content of a cup and note it down on a piece of paper.
- Evaluation and documentation: end of the day, the caregiver manually sums up all registered volumes, decides if hydration is sufficient and files the table which was used for documentation.
-> We need a sensor device, that automatically measures the drunk volume. To reduce errors (e.g. spilling), it would be best to do so as close to the process of drinking as possible.
-> The measured data should be analyzed and processed automatically. The human should only be needed to act if the hydration level is low.
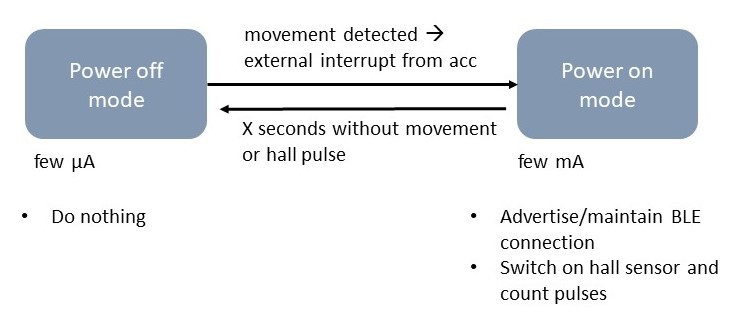
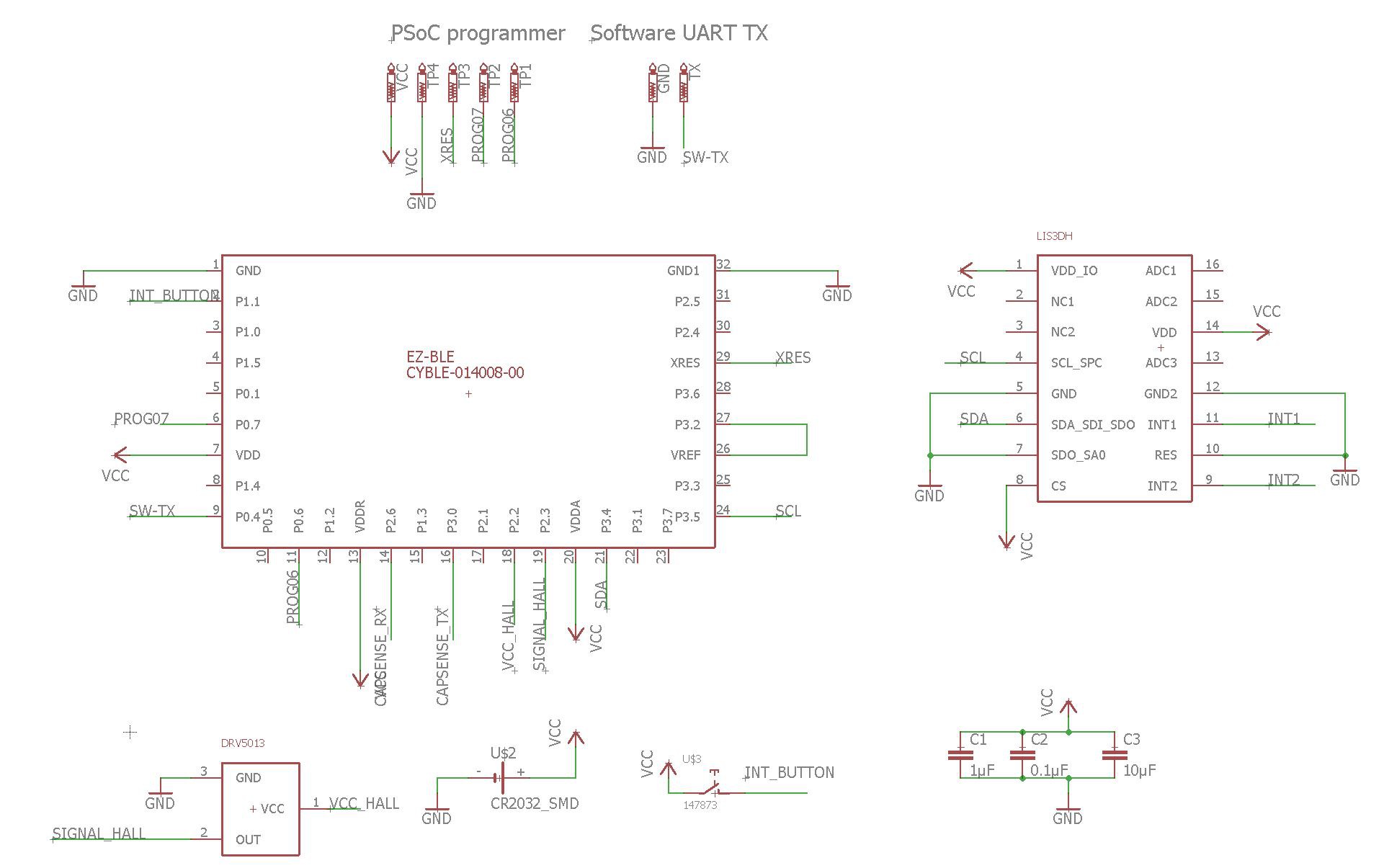
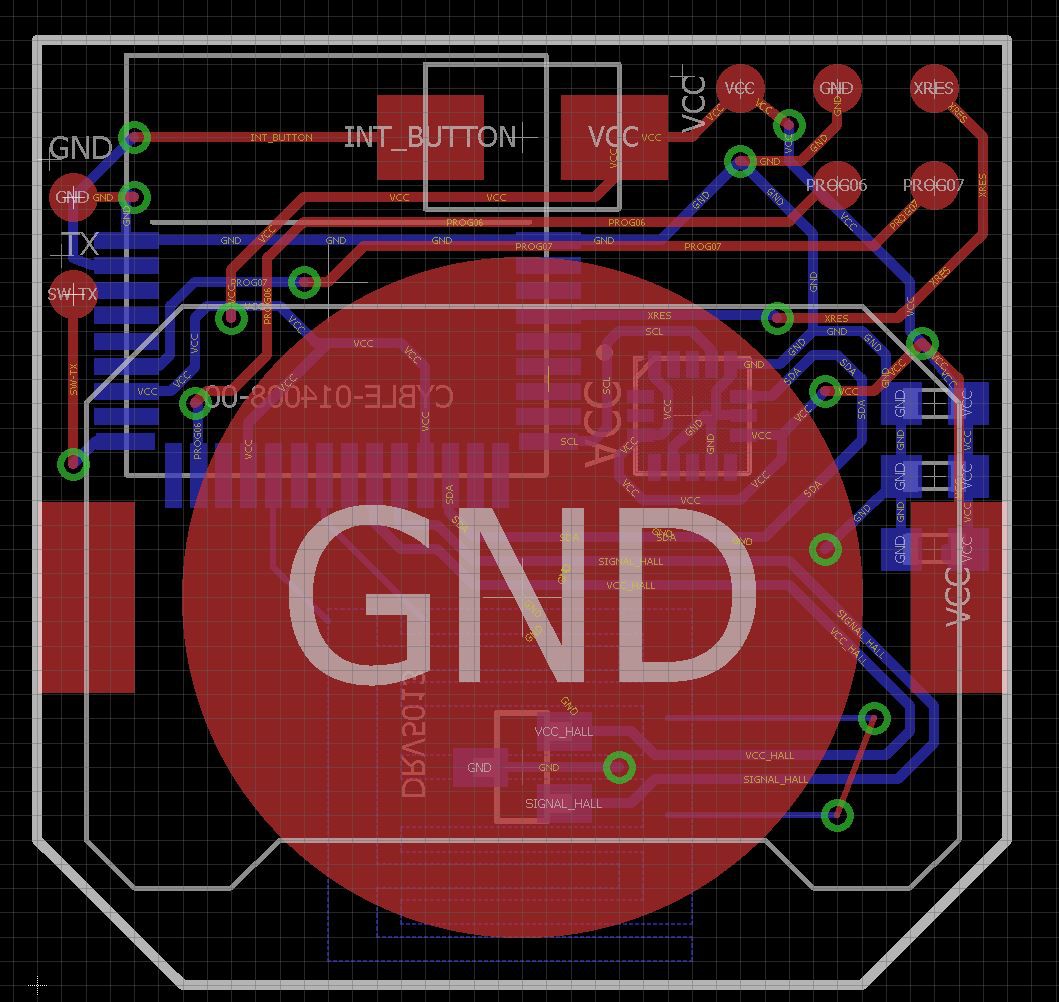
With these two points and the requirements in mind, the following architecture seems legit:
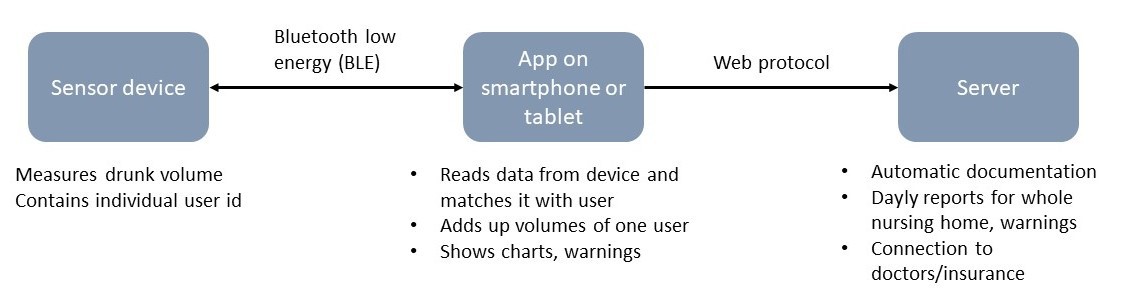
Intended way of use
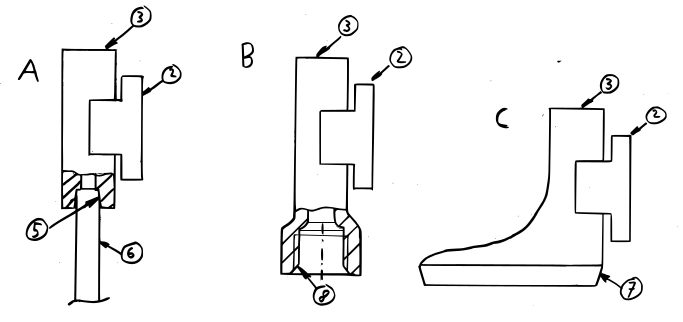
- When preparing drinks, the caregiver in the nursing home fits a suitable version of the mouthpiece to the drinking container. The mouthpiece comes in different forms: e.g. the tip for a regular straw, the lid of a feeding cup or the screw cap for a coke bottle.
- When handed the drink, the individual clicks in her/his personal sensor unit. Now, the assembly measures the volume he/she drinks and saves the value within the sensor unit.
- When finished, the sensor unit is detached from the mouthpiece and remains at the individual. The mouthpiece is collected and put into the dishwasher, with many others.
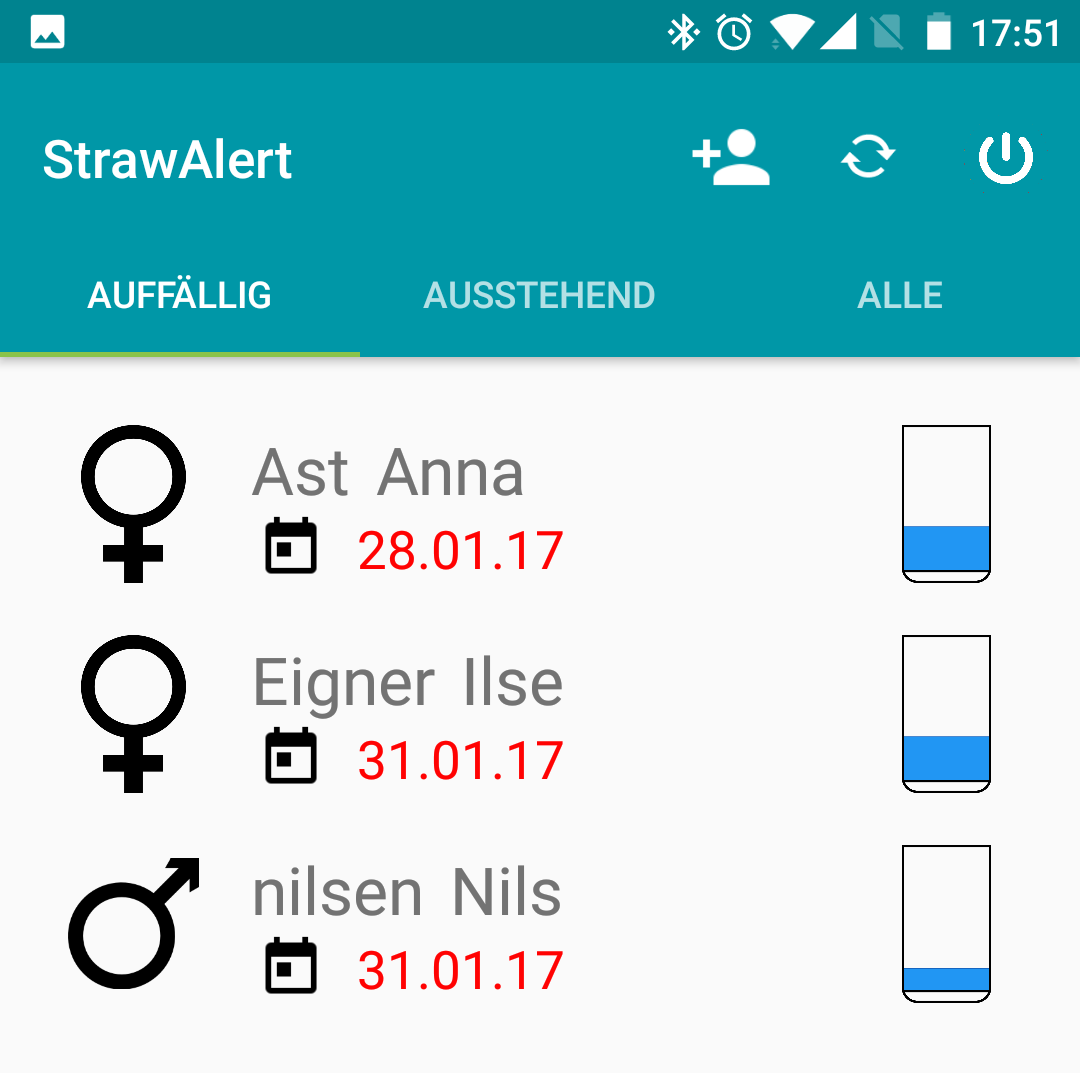
- In the end of the day, a nurse walks by with a phone or tablet, which automatically collects all the data saved on the sensor units, pops up warnings if neccessary and hands over the data for automatic documentation
![]()
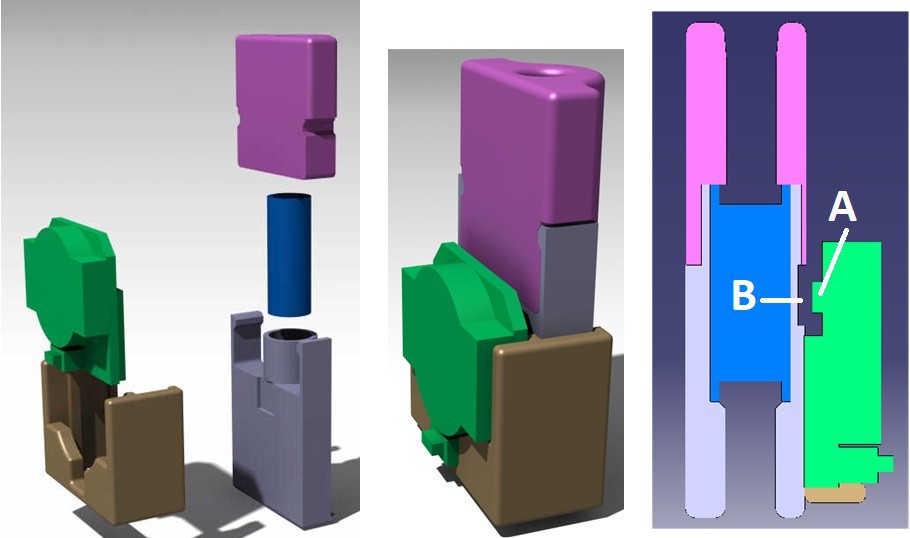
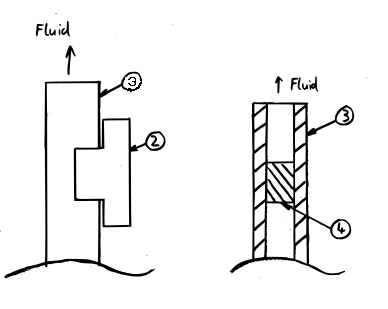
Example of use: mouthpiece (1) with attached sensor unit (2) mounted on a regular straw
Additional requirements
- Compact: The sensor device is small enough to be added to everyday drinking equipment
- Usable: everybody’s grandma should be able to use the device.
- Affordable: no expensive medTech product. Affordable for everyone!
- Modular: the device is not be limited to only one cup or bottle. It is possible to use it with the different containers we use when drinking every day.
- Robust: the...
 jflaschberger
jflaschberger


























 Curt White
Curt White
 Rohan Menon
Rohan Menon
 Kris Winer
Kris Winer
 Vignesh Ravichandran
Vignesh Ravichandran
Hey Nathan, thank you for the thumbs up! The bulkyness of the HydraCoach water bottle (and others, like the kickstarter-originated "Hidrate Spark") and the need to drink from these massive pieces of plastic for measurement are an ergonomic problem in itself.
In terms of your (wonderful!) offer of collaboration: actually my developement is a tiny bit more advanced than the documentation right now, so there will be more frequent updates in the next few weeks, when I have more time to type it down. I will have uploaded it all here within August. Let's collaborate from this stage on, then!